
Author: Hannah Goodings | Reviewer: Frédérique Courtois | Published: 11 September 2023 | Updated: ~
Key Points
- Women with spinal cord injuries (SCI) can have successful, safe, pregnancies.
- Along with the many changes that able-bodied pregnant women experience, there are unique risks for women with SCI during pregnancy, delivery and postpartum periods.
- Having regular communications with a team of medical professionals before, during and after pregnancy can help ensure a safe pregnancy for the mother and the child.
Yes. Female fertility is often unaffected after SCI meaning that women with SCI are able to have successful pregnancies. During the initial phase of recovery, the majority of women experience a menstruation pause lasting 5-12 months. Once menstruation resumes, the women’s ability to undergo pregnancy returns to normal.
Refer to SCIRE Professional’s module on Sexual and Reproductive Health for more information!
It is recommended that women with SCI attend a consultation prior to pregnancy to discuss the unique risks involved when pregnant with SCI. This conversation and continued appointments with health care professionals during pregnancy can help ensure a safe pregnancy, delivery and postpartum period. Common preconception medical team members may include:
Obstetrician
A skilled medical professional who specializes in pregnancy and births. Finding an obstetrician with SCI expertise can be greatly beneficial as they may have adapted medical equipment and experience detecting specific SCI pregnancy risks and warning signs.
Midwife
A health professional who often works with women pre-conception, during pregnancy, during delivery and after birth, often in collaboration with other hospital medical staff. It should be noted that the role of midwives varies around the globe.
Obstetric anesthesiologist
A trained anesthesiologist who specializes in epidurals during delivery. An epidural is frequently used for pain reduction but in SCI populations can also reduce the risk of autonomic dysreflexia occurring during birth. For this reason, an obstetric anesthesiologist with SCI expertise is beneficial.
Spinal nurse
A nurse that specializes in SCI care, both acutely and long-term.
Physical/Occupational Therapist
Therapists who create mobility programs and adjusted techniques of completing activities of daily living and exercises in a safe manner.
Meeting with multiple practitioners can be time consuming. Finding a team with strong communication between health care providers can ease some of this.
Women with SCI are able to have healthy pregnancies and births. However, these pregnancies are often considered high risk due to the added SCI related risks during pregnancy. These include:
Bladder and Bowel
Urinary Tract Infections (UTI)
UTIs are a common issue after SCI and may require antibiotic treatment. Pregnancy can reduce your mobility and put more pressure on your bladder, increasing the risk of incontinence and put you at higher risk of developing a UTI. Some women may choose to use an for all or the later portion of pregnancy to help with incontinence issues. Catheters can be useful for greater bladder control, but they also pose a risk for infection. Proper catheter hygiene and monitoring of symptoms is important to catch UTIs early.
Kidney Stones
Individuals with SCI are at higher risk of developing kidney stones due to incomplete bladder emptying, use of catheters, or neurogenic bladder conditions. During pregnancy, this risk increases due to decreased mobility and the potential for increased incontinence. If you experience fever, frequent UTI symptoms, or pain (though not all individuals with SCI will experience pain) consult your health care provider to determine the best course of action.
Autonomic Dysreflexia
Autonomic dysreflexia (AD) can be triggered by a full bladder or constipation. During pregnancy, the risk for bladder incontinence and constipation increases. This risk can be reduced with a schedule and tracking system for urinary and bowel movements. Speaking to a registered dietitian to adjust fiber intake or begin laxatives may also be helpful to decrease constipation risk.
Refer to our articles on Bladder Changes, UTIs, and Autonomic Dysreflexia for more information!
Spasticity
 For some individuals, spasticity worsens during pregnancy. Medication use during pregnancy, particularly spasticity-reducing medication, should be discussed with a physician to keep both the mother and child safe.
For some individuals, spasticity worsens during pregnancy. Medication use during pregnancy, particularly spasticity-reducing medication, should be discussed with a physician to keep both the mother and child safe.
| Some common medications, taken by individuals with SCI (for pain, spasticity etc.) may negatively affect the baby if taken during pregnancy. Consulting your family doctor to discuss medication options is crucial. |
Pressure Injuries
 Reduced mobility and increased weight gain during pregnancy both play a role in the increased likelihood of pressure injuries developing. Regular pressure adjustments, skin assessments and chair fittings, completed by a seating specialist, should be done to avoid pressure injury complications during the pregnancy.
Reduced mobility and increased weight gain during pregnancy both play a role in the increased likelihood of pressure injuries developing. Regular pressure adjustments, skin assessments and chair fittings, completed by a seating specialist, should be done to avoid pressure injury complications during the pregnancy.
Refer to our articles on Spasticity and Pressure Sores for more information!
Mobility and Fatigue
 Weight gain, increased abdominal pressure and increased spasticity during pregnancy can lead to decreased mobility and fatigue. Sleep quality is also commonly impacted by pregnancy and can worsen existing fatigue. This may result in needing help completing tasks that you have been independent in before pregnancy. It is important to pay attention to tasks you may need help with during pregnancy to ensure you have the correct supports in place.
Weight gain, increased abdominal pressure and increased spasticity during pregnancy can lead to decreased mobility and fatigue. Sleep quality is also commonly impacted by pregnancy and can worsen existing fatigue. This may result in needing help completing tasks that you have been independent in before pregnancy. It is important to pay attention to tasks you may need help with during pregnancy to ensure you have the correct supports in place.
Breathing
 In women with higher SCIs, breathing issues may be present or worsen during pregnancy. Raising the upper body on pillows when lying down can help with breathing but regular checks should be done to prevent pressure sores or skin shearing in this position. Those with tetraplegia may be at increased risk of pneumonia. For those with a weak cough, there is an increased risk of aspiration if experiencing vomiting from morning sickness that may be reduced by side lying. Speaking to a physiotherapist about breathing exercises or modifications to assisted coughing may also be helpful to improve breathing.
In women with higher SCIs, breathing issues may be present or worsen during pregnancy. Raising the upper body on pillows when lying down can help with breathing but regular checks should be done to prevent pressure sores or skin shearing in this position. Those with tetraplegia may be at increased risk of pneumonia. For those with a weak cough, there is an increased risk of aspiration if experiencing vomiting from morning sickness that may be reduced by side lying. Speaking to a physiotherapist about breathing exercises or modifications to assisted coughing may also be helpful to improve breathing.
Fetus Position
Fetal malpresentation, a condition where the fetus is not properly positioned, is more common in women with SCI due to decreased muscle tone within the abdominal wall. Routine ultrasounds should be conducted during pregnancy to check the fetus’ positioning to create a safe birth plan.
Pregnancy alters and stresses many systems in the body for both able-bodied women and women with SCI. Women with SCI have higher risks with the complications listed above and may need additional support to ensure healthy pregnancies. However, with the proper medical support, a successful and safe pregnancy can be achieved.
Having regular appointments and good communication within your medical team are both key to developing a safe and successful birth plan. During delivery, some SCI specific complications to be aware of include:
Being unaware that labour has begun
Depending on the level of injury, contractions or fetal movements may not be felt by the mother. This has the potential to lead to an unexpected birth, which can be dangerous to both the newborn and the mother. To avoid this, regular cervical dilation checks should be completed from week 28 onward. For women with injury levels above T10, early hospitalization after week 36 may be recommended.
Autonomic dysreflexia
Autonomic dysreflexia (AD) is a risk throughout all the stages of pregnancy, but the risk is even more elevated during the time of labour and delivery. Some stimuli that may lead to AD include contractions and manipulation of the uterus, bladder or vagina, all involved in childbirth. AD leads to a sharp rise in blood pressure with symptoms such as a throbbing headache, red skin, nausea, and can be life threatening. The treatment for AD occurring during birth is to stop all manipulation and position the mother in an upright position. If AD cannot be controlled during birth, a caesarean section may be required to safely deliver the baby.
An epidural can reduce pain during delivery for some and it is also a valuable tool used to decrease the risk of AD. Because of its utility in decreasing the risk of AD, epidural injection may be recommended regardless of the mother’s ability to feel birthing pains. In particular, it is recommended that women with SCI above T6 should have an epidural catheter placed at T10. In some cases, an epidural may be difficult if the mother has had lumbar or thoracic spinal surgery in the past. If an epidural cannot be completed, a local anesthetic may be used before any birthing surgeries such as an episiotomy.
 With every pregnancy being unique, the decision of where to give birth requires a discussion with your medical team. If the mother’s injury level is below T6, safe delivery at a local hospital rather than traveling to a large centre may be possible if all those involved are properly trained on the specific risks associated with SCI during childbirth. This decision should be made with the medical team and mother to ensure a safe delivery.
With every pregnancy being unique, the decision of where to give birth requires a discussion with your medical team. If the mother’s injury level is below T6, safe delivery at a local hospital rather than traveling to a large centre may be possible if all those involved are properly trained on the specific risks associated with SCI during childbirth. This decision should be made with the medical team and mother to ensure a safe delivery.
In the past, women with SCI have often been advised that a caesarean section (C-section) is the safest option for childbirth. In some cases, where fetal positioning is incorrect or due to other complications, a C-section may be needed. However, in other cases, vaginal births can be safely completed in women with SCI. The discussion of vaginal or caesarean birth should be a conversation involving the mother and her medical team in order to best achieve a safe and successful birth.
After giving birth, most women with SCI have longer stays in hospitals compared to able-bodied women. This allows for continued care of bladder emptying, birthing wounds and monitoring. After discharge from the hospital, some complications that you may face as a mother with SCI include:
Wound Healing
Due to decreased or complete lack of sensation, birthing wounds for SCI patients must be carefully inspected often to ensure they are healing properly. Women may stay in the hospital to get the care needed or they may head home if wound care can be safely continued there. Daily wound cleaning should be completed until healing is complete. If possible, visits from a midwife or nurse may be beneficial during this time.
Breastfeeding

Watch SCIRE’s video explaining ways you can breastfeed with assistive aids.
Mothers with SCI often have the ability to breastfeed normally.
However, you may face some complications depending on your level of injury. Women with:
- injuries above T6 tend to have reduced milk production,
- injuries above T4 can experience trouble releasing milk due to reduced sensation of the baby latching onto the breast,
- any level of injury may have trouble positioning the baby or holding the baby for the entirety of feeding times. In these cases, breastfeeding pillows or laying down while feeding may be a good option.
If it is determined that the baby is not getting enough to eat through breastfeeding alone, supplemental formula may be advised.
Refer to our article on Breastfeeding for more information!
Mental Health
Following delivery, many women, both able-bodied and disabled, deal with mental health changes and some develop postpartum depression or anxiety. Individuals living with SCIs are at a higher risk of depression, leading to a higher rate of postpartum depression and anxiety.
Postpartum Depression
Postpartum depression can be described by a major episode of depression occurring within 12 months of giving birth. Following delivery, many women experience postpartum blues, associated with mood swings during the first 4-10 days. An important difference is that postpartum depression greatly affects activities of daily living and postpartum blues does not.
Postpartum Anxiety
Postpartum anxiety is a major episode of anxiety during the months following giving birth and is also thought to be a more common risk in SCI populations.
Both postpartum depression and postpartum anxiety can have negative effects on the mother, child and supporting family if not treated. If you know someone suffering from either of these conditions, encouraging them to seek help from a medical professional as soon as possible is crucial.
There are increased or unique pregnancy-related considerations for women with SCI such as pressure sores, mobility and fatigue issues, autonomic dysreflexia during childbirth, and issues around wound healing. However, women with SCI can have healthy pregnancies, deliveries and motherhoods, helped along with their medical team.
For a review of how we assess evidence at SCIRE Community and advice on making decisions, please see SCIRE Community Evidence.
SCIRE Community. Sexual Health After SCI. Available from: community.scireproject.com/topic/sexual-health/
SCIRE Community. Urinary Tract Infections. Available from: community.scireproject.com/topic/urinary-tract-infections/
SCIRE Community. Breastfeeding. Available from: community.scireproject.com/videos/breastfeeding/
SCIRE Professional. Sexual Reproductive Health: scireproject.com/evidence/sexual-and-reproductive-health/introduction/
SCIRE Community. Autonomic Dysreflexia. Available from: community.scireproject.com/topic/autonomic-dysreflexia/
SCI BC. Breastfeeding After SCI. Available from: https://sci-bc.ca/breastfeeding-after-sci/
SCI BC. Female Fertility and Pregnancy. Available from: https://scisexualhealth.ca/female-fertility-and-pregnancy/
References presented in order they appear in text.
Robertson, K., & Ashworth, F. (2022). Spinal cord injury and pregnancy. In Obstetric Medicine (Vol. 15, Issue 2, pp. 99–103). SAGE Publications Inc. https://doi.org/10.1177/1753495X211011918
Welk, B., Fuller, A., Razvi, H., & Denstedt, J. (2012). Renal stone disease in spinal-cord–injured patients. Journal of endourology, 26(8), 954-959. https://doi.org/10.1089/end.2012.0063
Wendel, M., Whittington, J., Pagan, M., Whitcombe, D., Pates., McCarthy, R., Magann, E. (2021). Preconception, Antepartum, and Peripartum Care for the Woman with a Spinal Cord Injury: A Review of the Literature. Obstertrical and Gynecological Survery. https://pubmed.ncbi.nlm.nih.gov/33783544/
Bertschy, S., Schmidt, M., Fiebag, K., Lange, U., Kues, S., & Kurze, I. (2020). Guideline for the management of pre-, intra-, and postpartum care of women with a spinal cord injury. Spinal Cord, 58(4), 449–458. https://doi.org/10.1038/s41393-019-0389-7
Stoffel, J. T., van der Aa, F., Wittmann, D., Yande, S., & Elliott, S. (2018). Fertility and sexuality in the spinal cord injury patient. World Journal of Urology, 36(10), 1577–1585. https://doi.org/10.1007/s00345-018-2347-y
Spinal Outreach Team (2017). The impact of a spinal cord injury on pregnancy, labour and delivery: What you need to know, Brisbane, Queensland: Queensland Health. https://www.health.qld.gov.au/__data/assets/pdf_file/0027/425772/pregnancy-sci.pdf
Robertson, K., Dawood, R., & Ashworth, F. (2020). Vaginal delivery is safely achieved in pregnancies complicated by spinal cord injury: A retrospective 25-year observational study of pregnancy outcomes in a national spinal injuries centre. BMC Pregnancy and Childbirth, 20(1). https://doi.org/10.1186/s12884-020-2752-2
Crane, D. A., Doody, D. R., Schiff, M. A., & Mueller, B. A. (2019). Pregnancy Outcomes in Women with Spinal Cord Injuries: A Population-Based Study. PM and R, 11(8), 795–806. https://doi.org/10.1002/pmrj.12122
Bertschy, S., Bostan, C., Meyer, T., & Pannek, J. (2016). Medical complications during pregnancy and childbirth in women with SCI in Switzerland. Spinal Cord, 54(3), 183–187. https://doi.org/10.1038/sc.2015.205
Lee, A. H. X., Wen, B., Walter, M., Hocaloski, S., Hodge, K., Sandholdt, N., Hultling, C., Elliott, S., & Krassioukov, A. v. (2021). Prevalence of postpartum depression and anxiety among women with spinal cord injury. Journal of Spinal Cord Medicine, 44(2), 247–252. https://doi.org/10.1080/10790268.2019.1666239
Kroska, E. B., & Stowe, Z. N. (2020). Postpartum Depression: Identification and Treatment in the Clinic Setting. In Obstetrics and Gynecology Clinics of North America (Vol. 47, Issue 3, pp. 409–419). W.B. Saunders. https://doi.org/10.1016/j.ogc.2020.05.001
Image credits
- Medical team Cromaconceptovisual CC0
- Excretory system ©Olena Panasovska, CC BY 3.0 US
- Digestive System ©Design Science, CC0 1.0
- Medication CC BY 3.0 US
- Pressure Injuries CC BY 3.0 US
- Help CC BY 3.0 US
- Breathing CC BY 3.0 US
- Fetus position CC BY 3.0 US
- Pregnant ©Luis Prado CC BY 3.0 US
- Voltage ©Clker-Free-Vector-Images, CC0 1.0
- Hospital Public Domain © Public Domain Certification
- Breastfeeding © SCIRE Community Team
- Mental Health ©Loritas Medina CC BY 3.0 US


 It is accepted that breast milk (colostrum, transitional milk and mature milk) is the first choice to help your baby grow and develop. The benefits for your baby include:
It is accepted that breast milk (colostrum, transitional milk and mature milk) is the first choice to help your baby grow and develop. The benefits for your baby include: Women with SCI, just like women without SCI, are encouraged to give breastfeeding a try. By trying, you can then see how it works for both you and for your baby. If breastfeeding does not work well, there are several safe and healthy options available to you to ensure both your needs and your baby’s needs are met.
Women with SCI, just like women without SCI, are encouraged to give breastfeeding a try. By trying, you can then see how it works for both you and for your baby. If breastfeeding does not work well, there are several safe and healthy options available to you to ensure both your needs and your baby’s needs are met.

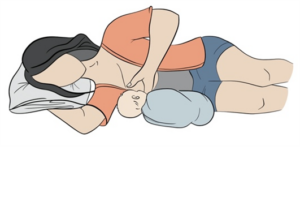

 Talk to your health care providers, including lactation consultant and paediatrician about the most safe and effective options for feeding your baby, as well as medications for you and your baby.
Talk to your health care providers, including lactation consultant and paediatrician about the most safe and effective options for feeding your baby, as well as medications for you and your baby. Many effects of medications on breastfeeding babies simply are not known. Due to this, only take a medication when absolutely needed, at the lowest dose, and for the shortest time possible.
Many effects of medications on breastfeeding babies simply are not known. Due to this, only take a medication when absolutely needed, at the lowest dose, and for the shortest time possible.
 Bonding, or what is often called ‘attachment’ or the ‘caring connection’ between a child and parent, is an important part of a child’s physical and emotional development. Some parents report immediately feeling a strong connection with their child during pregnancy or soon after the birth. Other parents report they did not feel an instant connection. Both feelings are okay and normal.
Bonding, or what is often called ‘attachment’ or the ‘caring connection’ between a child and parent, is an important part of a child’s physical and emotional development. Some parents report immediately feeling a strong connection with their child during pregnancy or soon after the birth. Other parents report they did not feel an instant connection. Both feelings are okay and normal. Why am I feeling so sad or anxious?
Why am I feeling so sad or anxious?